Neighbourhood Care in the Netherlands
Developing a good relationship with our patients helps us better appreciate and understand their environment. The treatment we can then implement empowers them through giving them autonomy over their condition.
In 2006, district nurses in the Netherlands were becoming increasingly dissatisfied with the model of care being provided to people with complex health needs in the community.
Traditional models utilized low cost, lesser trained personnel to provide care. In response, the Buurtzorg (Dutch for ‘Neighbourhood Care’) care model was established. The model consists of the recruitment of highly skilled nursing professionals working in independent teams of up to 12 nurses) taking responsibility within a defined area of all aspects of care of 50-60 patients.
The model relies on IT systems for online scheduling, documentation of nursing assessments and billing. The Neighbourhood Care model aims to:
- Create self-governing teams of nurses to provide both medical and supportive home care services
- Become a sustainable, holistic model of community care
- Maintain or regain patients’ independence
- Train patients and families in self-care
- Create networks of neighborhood resources
- Rely on the professionalism of nurses
In 2015, Buurtzorg employed 8,000 nurses in 700 teams, providing a full range of medical and support services to over 65,000 patients.
At the heart of the nurse-led model is client empowerment; by making the most of the clients’ existing capabilities, resources and environment and emphasizing self-management the teams garnered highly successful results.
The scheme reduced clients’ costs by 40%, saving a potential of 2 billion euros per year and reducing the hours of care per patient by 50%. Quality of care was also improved as the patients regained autonomy more quickly, fewer hospital admissions were recorded as well asshorter lengths of stays.
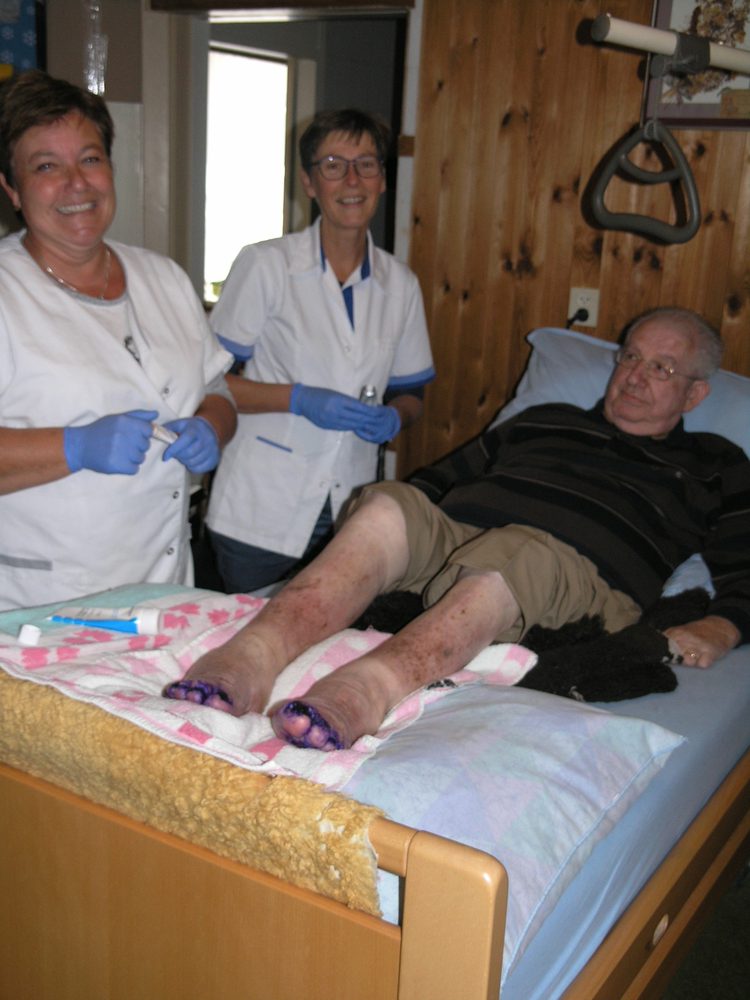
Ornella Zanin and Gerda Mast, District Nurses specialized in triage of chronic wounds, shared this story to illustrate the strength of the programme.
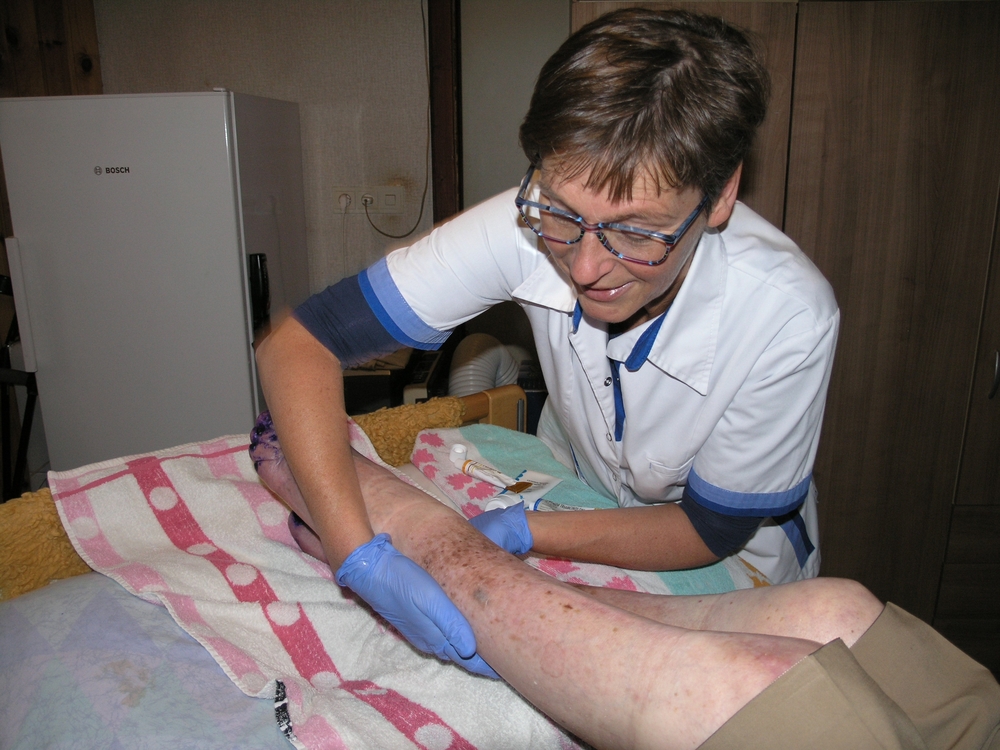
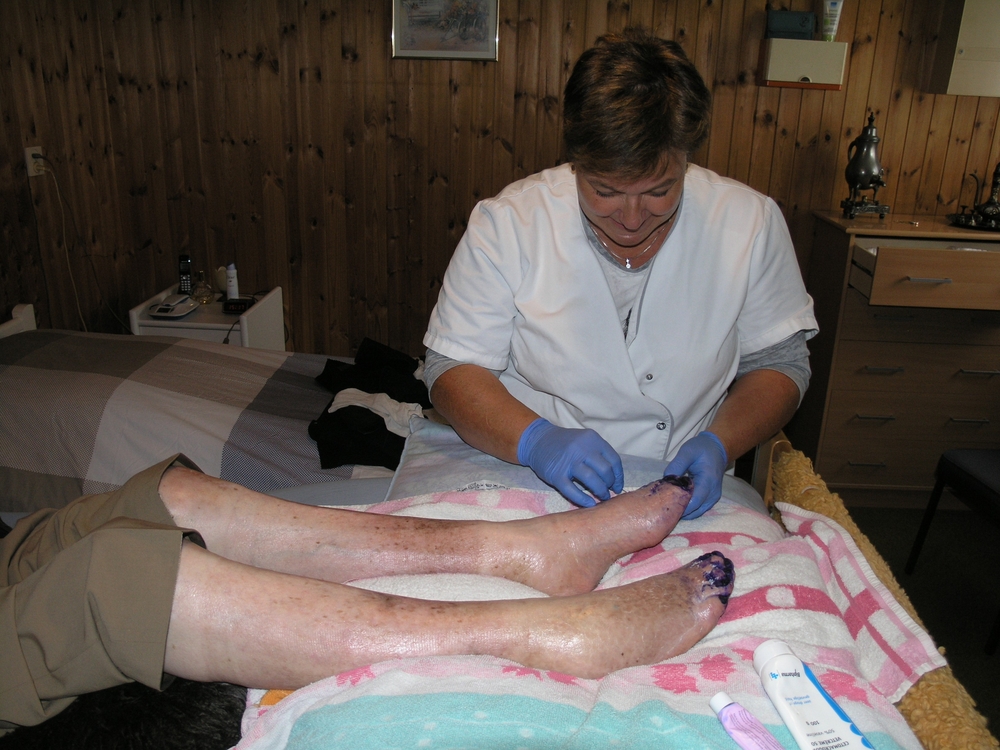
Lars, a 70 year old man resident in one of the neighbourhoods served by Buurtzorg was in need of a serious intervention. Wheelchair-bound after being infected by polio as a child and suffering from Guillain-Barre syndrome, he contracted an ulcer on his lower right leg, subsequently complicated by mycosis which spread to the leg and toes. The pain prevented compression therapy leading to significant leg edema. Lars was largely confined by his condition, unable to appropriately care for his legs and feet, and was also resistant to varying forms of treatment.
Ornella and Gerda visited Lars in his house and worked together with him to develop a treatment plan for his wound. Within six weeks, the wound was healed. Through developing a good relationship with Lars and appreciating a better understanding of his environment, Ornella and Gerda were able to implement a treatment plan that was not only successful in the short term, but has also led to the empowerment of Lars so that he is more attentive in the care of his legs.
References
Belardi, L. (2014). “Dutch model offers new approach to home care.” Retrieved 7 November, 2016, from http://www.australianageingagenda.com.au/2014/07/30/dutch-model-offers-alternative-approach-home-care/
The Commonwealth Fund (2015). “Home Care by Self-Governing Nursing Teams: The Netherlands’ Buurtzorg Model.” Retrieved 7 November, 2016, from http://www.commonwealthfund.org/publications/case-studies/2015/may/home-care-nursing-teams-netherlands